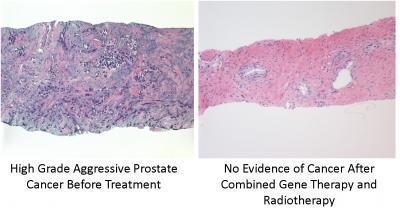
HOUSTON, Dec. 12 (UPI) — When combined with chemotherapy, a treatment called “suicide gene therapy” successfully and safely kills prostate tumor cells.
Suicide gene therapy is a gene modification strategy. A patient’s tumor cells are modified to trigger the body’s immune system to attack them.
Researchers at Houston Methodist Hospital used the combination to treat 66 prostate cancer patients between 1999 and 2003. The 66 patients were divided into two groups, based on the severity of their cancer. Less severe cases were treated with radiotherapy, while more severe cases warranted both radiotherapy and hormonal therapy.
Both groups of patients also received suicide gene therapy. Less severe cases received the therapy twice over the course of the study, while more severe cases were treated three times.
Both groups of patients fared well. The less severe group of patients boasted a survival rate of 97 percent. Patients with more severe cancer had a 94 percent survival rate.
The survival rate results were 5 to 20 percent better than survival rates achieved by current procedures.
Researchers at the Houston hospital are able to manipulate the prostate cancer cells using a combination of viruses. An adenovirus, like the virus that causes the common cold, is used to deliver a a herpes virus gene directly into the cells.
“Once the herpes virus gene was delivered and it started manufacturing TK [thymidine kinase], we gave patients a commonly used anti-herpes drug, valacyclovir,” Brian Butler, chair of the radiation oncology department at Houston Methodist, said in a press release. “The combination attacked the herpes DNA, and the TK-producing tumor cells self-destructed, which is why the procedure is called ‘suicide gene therapy.'”
The strategy also works to clue the body’s immune system to the presence of the tumor cells, and encourages a more comprehensive attack.
“We have created a vaccine with the patient’s own cancer cells, a treatment that complements, and may even enhance, what we can achieve with traditional radiation and hormonal therapies,” added Butler.
Researchers, who published their findings in the Journal of Radiation Oncology, believe the treatment combination could soon become common practice.
“This is extremely pleasing to us, considering we had patients enrolled in our protocol after other physicians deemed them incurable,” said lead study author Bin Teh, vice chair of radiation oncology. “We firmly believe this will be a viable treatment strategy.”






