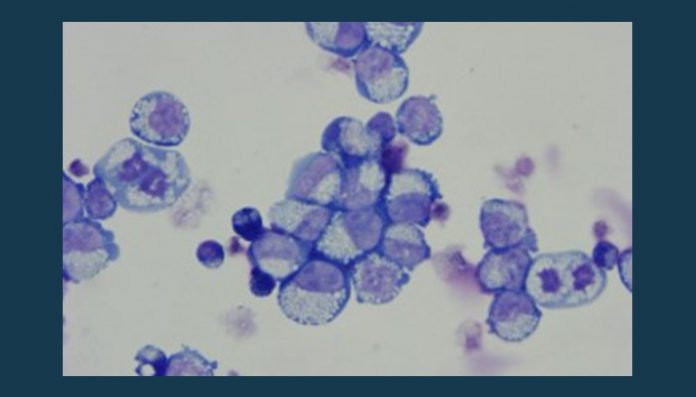
March 25 (UPI) — Researchers at the University of Bristol in England have created the first immortalized blood cell lines, allowing for the mass production of red blood cells.
The team of researchers collaborated with NHS Blood and Transplant to create large-scale manufactured red blood cells, which could lead to a safe source of transfusions for people with rare blood types and to compensate for blood donation shortages.
Previous studies have involved growing donated stem cells into mature red blood cells, but this method produces only small numbers of mature cells and requires repeated donations.
“Previous approaches to producing red blood cells have relied on various sources of stem cells which can only presently produce very limited quantities,” Dr. Jan Frayne, of the University of Bristol’s School of Biochemistry, said in a press release. “By taking an alternative approach we have generated the first human immortalized adult erythroid line [Bristol Erythroid Line Adult or BEL-A], and in doing so, have demonstrated a feasible way to sustainably manufacture red cells for clinical use from in vitro culture. Globally, there is a need for an alternative red cell product. Cultured red blood cells have advantages over donor blood, such as reduced risk of infectious disease transmission.”
Immortalized cells are created by trapping stem cells at the early stage to generate a stable line so they grow indefinitely and can be triggered to become red blood cells.
“Scientists have been working for years on how to manufacture red blood cells to offer an alternative to donated blood to treat patients,” Dave Anstee, director at the NIHR Blood and Transplant Research Unit in Red Cell Products, said. “The first therapeutic use of a cultured red cell product is likely to be for patients with rare blood groups because suitable conventional red blood cell donations can be difficult to source.
“The patients who stand to potentially benefit the most are those with complex and life-limiting conditions like sickle cell disease and thalassemia, which can require multiple transfusions of well-matched blood. The intention is not to replace blood donation but provide specialist treatment for specific patient groups,” Anstee added.
Researchers said it would be many years before manufactured cells would be available on a large scale.
The study was published in Nature Communications.